Recently, a friend received a lot of triple-negative breast cancer patients sent to the questions on female cancer prevention fund public micro-channel number, the staff conducted a lot of meticulous combing, and today we chat with triple negative breast cancer substantially knowledge and the latest advances in clinical treatment, we hope to triple negative breast cancer patients and their families to provide a reference value.
 What is triple negative breast cancer?
What is triple negative breast cancer?
Often heard friends say the medical profession in particular treat triple negative breast cancer, triple negative breast cancer can not help but wonder really so terrible? First, let us take a look at what is triple-negative breast cancer.
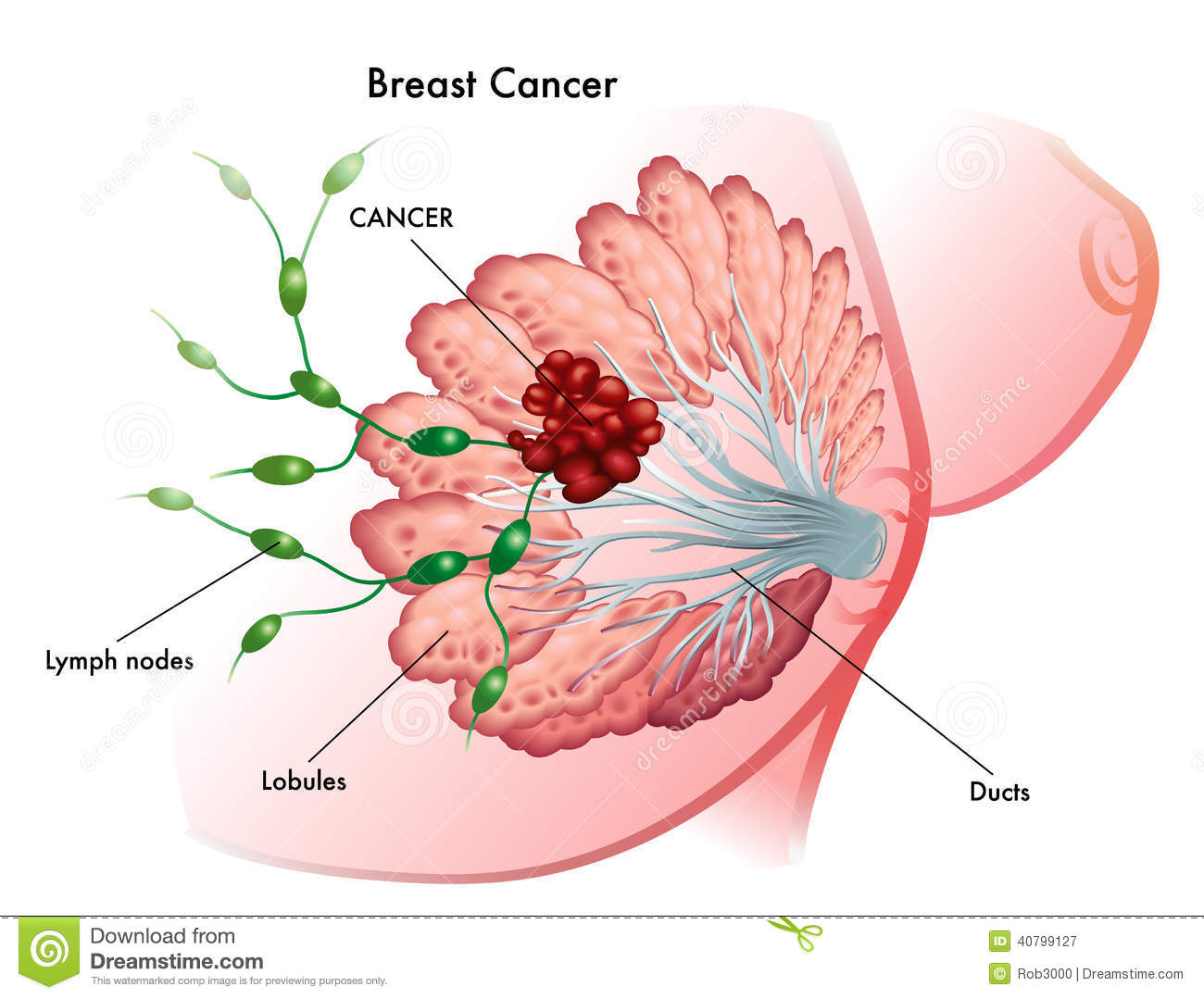
Breast cancer is divided into various subtypes, triple negative breast cancer (triple negative breast cancer, TNBC) refers to the estrogen receptor (ER), progesterone receptor (PR) and human epidermal growth factor receptor 2 (Her-2 ) a breast cancer were negative. Clinical data show that triple negative breast cancer accounts for all types of breast cancer pathology 15% -23.8%.
Triple negative breast cancer is considered to be the type of breast cancer in the most dangerous, with strong invasion, is characterized by high degree of malignancy, and visceral metastasis and local recurrence rate, its main site of distant metastasis to bone, lung, liver , brain; at the same time, triple negative breast tumors larger, high histological grade, pathological type usually invasive ductal carcinoma, the patient’s survival time is often shorter.
Triple negative breast cancer refractory Why?
Estrogen receptor (ER), progesterone receptor (PR) and human epidermal growth factor receptor 2 (Her-2) is a common and common to see three symbols on breast cancer pathology report, for the majority of breast cancer patients it is due to the body’s over-expression of ER and PR (positive) caused. If breast cancer is due to clear both receptor-positive due to the receptor can be suppressed by overexpression of mature endocrine therapy, to treat breast cancer, the prognosis is better.
Human epidermal growth factor is a piece of a strong promotion of various epidermal tissue cell growth gene, Her-2-positive means that overexpression of this gene, prone to excessive proliferation of a variety of skin tissue, becoming tumors. Although Her-2 positive breast cancer have invasive strong, more likely to relapse and metastasis, short disease-free survival characteristics, but there is now excellent treatment target drug “Herceptin”, earlier treatment , the greater the benefit.
Compared with non-triple negative breast cancer, triple negative breast cancer is currently no effective treatment for endocrine therapy and molecular targeted therapy are ineffective, so that treatment face great confusion, a kind of aimless frustration. Compared with other types of breast cancer, triple negative breast cancer treatment is relatively simple, mainly rely on chemotherapy; but if only conventional standard treatment, the prognosis is still very poor, relatively low recurrence-free survival and overall survival rates.
Triple negative breast cancer really can not do anything right?
Breast cancer is the highest incidence of cancer of the female Chinese, Chinese new cases of breast cancer each year about 249,000; according to scaling, it means that China had approximately 50,000 new cases of triple negative breast cancer each year. For these unfortunate triple-negative breast cancer patients, in addition to as “mouse”, as another round of chemotherapy to experiment with different combinations of programs to seek treatment outside really do anything yet?
I remember Mr. Feng Jicai wrote this sentence:. “Wind can blow a large sheet of white paper, but not blown away by a butterfly, the life force that disobedience” True to his word, domestic and foreign scientists and numerous tumors of cancer patients, also convinced that the true meaning of life is not compromised. To combat triple negative breast cancer, more and more scientists began to seek a breakthrough from the genetic level, depth molecular characterization of the biological triple negative breast cancer, may find new therapeutic targets, to improve treatment and improve the prognosis may have important clinical significance.
Breast cancer susceptibility gene BRCA1 / 2 is now confirmed tumor suppressor gene associated with hereditary breast cancer, BRCA1 / 2 gene mutation risk of breast cancer by up to 80%. Scientists have found that triple negative breast cancer in BRCA gene mutation rate of 10% -20% of the TNBC carry the BRCA mutation; wherein 57-80% of BRCA1 mutations in breast cancer and 23-35% of BRCA2 mutations in breast cancer is TNBC , suggesting that BRCA mutations TNBC patients may be able to find treatment for targeted drug BRCA genes.
Decoding triple negative breast cancer, help treatment, family benefits
April 6, 2015 study published in the “Journal of Clinical Oncology” in an attempt to identify those with metastatic triple negative breast cancer are expected to benefit in the platinum-based adjuvant chemotherapy (mTNBC) patients. This study selected patients mTNBC, let every 3 weeks to accept a first- or second-line cisplatin or carboplatin, including BRCA1 / 2 mutation carriers. A total of 86 patients received cisplatin (n = 43) or carboplatin (n = 43) treatment, the experimental results showed that germline BRCA1 / 2 mutation carriers (n = 11), showed higher pathologic complete response.
Such experimental results indicate that platinum drugs for mTNBC patients, especially the presence of germ cells BRCA1 / 2 mutation patients can prolong disease-free survival time and improve quality of life. This means that the BRCA gene testing is necessary for patients with TNBC, if identified as BRCA positive TNBC, patients can get a clear medication guide for the first time, do not become a “accompany treatment,” the victim, so not only can significantly reduce the chemotherapy drugs harm the body, but also can reduce the patient’s psychological pressure, increased disease-free survival time and improve the quality of life of patients, but also will significantly reduce the financial burden of patients.
BRCA genetic testing not only for the treatment of TNBC patients have a clear guiding value for the family members of patients with more aggressive prevention guidance value. Because breast cancer has obvious hereditary, BRCA1 / 2 gene deleterious mutations can be inherited from either the father or the mother, genetic carriers of deleterious mutations to their children probability is 50%. Therefore, if the family members of patients with breast cancer through genetic testing found himself carrying BRCA1 / 2 gene mutations harmful, they can be differentiated themselves from the general population, to take early targeted preventive measures to effectively control and reduce their risk of breast cancer.
Perhaps, in the not too distant future, BRCA genetic testing will and ER, PR, Her-2, as was listed as necessary for detecting breast cancer diagnosed before the index!