People genetically predisposed to have high blood pressure may be at lower risk for Alzheimer’s disease, according to a new study, though the researchers say this association is likely down to antihypertensive medication rather than the condition itself.
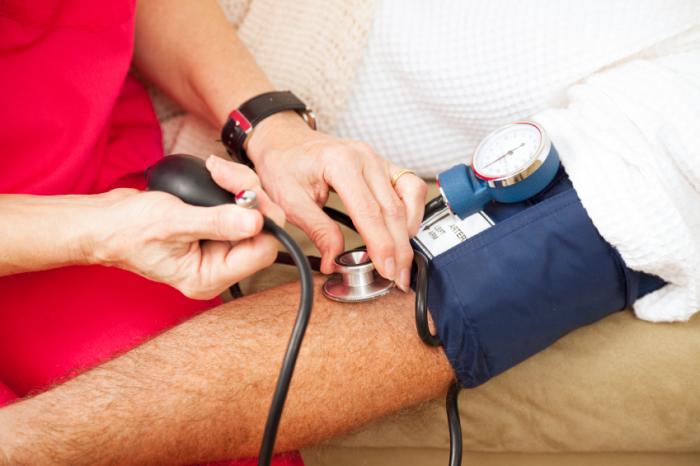
Researchers found people genetically predisposed to have high blood pressure may be at lower risk of Alzheimer’s, though antihypertensive drugs may be a likely driver rather than the condition itself.
Study co-author John Kauwe, associate professor of biology at Brigham Young University in Provo, UT, and colleagues publish their findings in the journal PLOS Medicine.
In the US, it is estimated that around 5.3 million people of all ages have Alzheimer’s disease – the most common form of dementia – with the number of cases expected to rise by 40% over the next 10 years.
Alzheimer’s is the sixth-leading cause of death in the US, with around 700,000 people aged 65 and older expected to die of the disease this year. It is the only cause of death in the top 10 that cannot be prevented, cured or slowed.
Prof. Kauwe and colleagues note that researchers are currently working to identify risk factors for Alzheimer’s, particularly ones that can be modified. “If such risk factors exist,” they add, “it might be possible to limit the predicted increase in future Alzheimer’s disease cases.”
Antihypertensive drugs should be investigated for Alzheimer’s prevention
With the aim of identifying modifiable Alzheimer’s risk factors in their study, the team analyzed data from the Alzheimer’s Disease Genetics Consortium and the International Genomics of Alzheimer’s Project, involving 17,008 people with Alzheimer’s and 37,154 people without the condition.
The researchers used a “supercomputer” to analyze the genomes of each participant, looking for single nucleotide polymorphisms (SNPs) – common genetic variations – that may be associated with potentially modifiable risk factors for Alzheimer’s, such as obesity, diabetes, high blood pressure and smoking.
“This is to date the most authoritative paper looking at causal relationships between Alzheimer’s disease and these potentially modifiable factors,” says Prof. Kauwe. “In terms of the number of samples, it can’t get bigger at this point.”
The team found that people who were genetically predisposed to have high systolic blood pressure were at lower risk for developing Alzheimer’s, compared with people who did not have a genetic predisposition for high blood pressure.
The researchers also found that individuals with genetically predisposed high blood pressure were much more likely to be using antihypertensive medication, causing the researchers to speculate it may be the use of these drugs rather than high blood pressure itself that drives this association.
Prof. Kauwe adds:
“It’s likely that this protective effect is coming from antihypertensive drugs. These drugs are already FDA [Food and Drug Administration] approved. We need to take a serious look at them for Alzheimer’s prevention.”
Since high blood pressure is a major risk factor for cardiovascular disease, the team warns against raising blood pressure as a preventive strategy for Alzheimer’s, “yet these findings offer intriguing etiological insight,” they add.
The researchers also identified a weak link between smoking quantity and lower risk of Alzheimer’s, though they note further studies are required to gain a better understanding of this association.
“Such analyses would address the causality of smoking as a risk factor, and offer valuable insight into nicotine’s role in the etiology of Alzheimer’s disease,” they explain. “Since smoking is a major cause of global disease burden, increasing knowledge of the role of nicotine in the etiology of Alzheimer’s disease may prove to be the more actionable insight.”
Earlier this month, Medical News Today reported on a study in which researchers discovered a blood protein that could predict an individual’s risk of Alzheimer’s.
Written by Honor Whiteman