In fertility preservation, reproductive tissues are saved, so that a person may have a child in the future. It usually involves freezing and storing eggs, sperm, or embryos, although other methods may be employed.
Men and women can preserve their fertility if they wish to delay parenthood, or if they are undergoing treatment for a medical condition such as cancer.
Contents of this article:
- How might cancer and cancer treatment affect fertility?
- Fertility preservation options for women
- Fertility preservation options for men
- Fertility preservation options for children with cancer
- Effects of fertility preservation on cancer treatment
How might cancer and cancer treatment affect fertility?
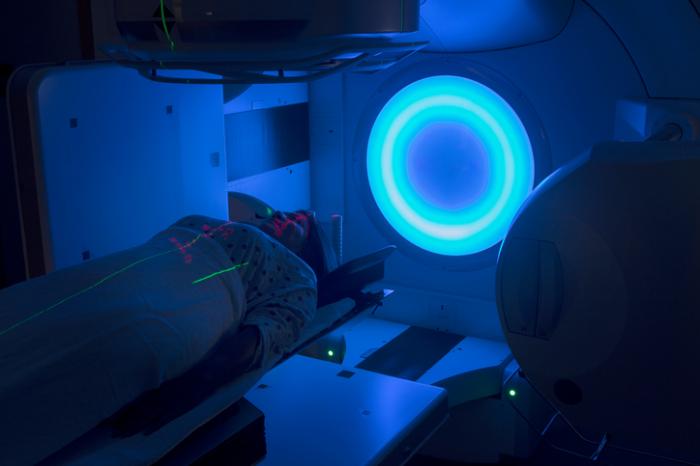
For females, radiation therapy may damage the eggs, ovarian follicles, and hormones.
Infertility is defined as the inability of a couple to conceive after at least 1 year of regular intercourse without the use of contraception.
Cancers of the reproductive organs, such as uterine cancer or testicular cancer, may cause infertility.
Other cancers may not directly damage fertility or cause sterility, but treatments for these cancers can.
The effects of cancer treatment on fertility may be temporary or permanent. The outcome depends on the person’s age, the type of cancer treatment they are having, the type and stage of the cancer, and their fertility status before treatment.
Female fertility and cancer treatment
Both chemotherapy and radiation therapy can reduce female fertility. These treatments may damage the eggs, ovarian follicles, and hormones. Radiation directed to the ovaries or chemotherapy drugs called alkylating agents are most harmful to fertility.
Premature menopause, occurring before 40 years of age, can be a side effect of some cancer treatments, with the risk of occurrence increasing as women age.
Surgical removal of the uterus or both ovaries will lead to infertility.
Male fertility and cancer treatment
Surgical removal of the testicles can harm male fertility.
Certain types of chemotherapy and high doses of radiation therapy can kill the stem cells that produce sperm. These types of treatment may also lead to a reduction in the quality or quantity of sperm or damage sperm DNA.
In addition, some hormone therapies used in the treatment of prostate cancer and other cancers may reduce male fertility.
When to talk to a doctor
Anyone who is planning cancer treatment and who wishes to have a child in the future should discuss fertility preservation with their doctor.
The doctor can advise whether the cancer treatment that the patient is about to undergo is likely to lead to infertility. They may suggest the best fertility preservation options available to that person.
The best time to preserve fertility is before cancer treatment starts, as even one session of treatment may damage fertility.
Fertility preservation options for women
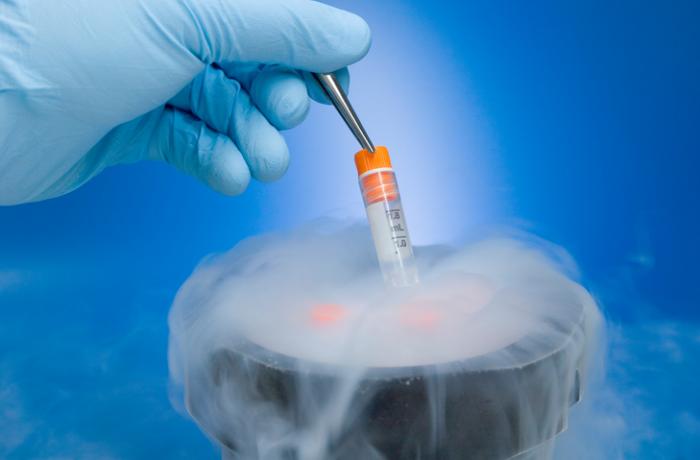
Embryo freezing is a common method of preserving female fertility.
Established methods of fertility preservation for women include:
- Ovarian transposition: One or both ovaries are surgically repositioned to protect them from radiation. This treatment is used for those women who are receiving radiation to an area other than the pelvic region. It does not offer complete protection, due to scatter radiation. If the woman still cannot conceive after the treatment, the ovaries may need to be moved again. In vitro fertilization (IVF) may also be necessary.
- Egg freezing, or oocyte cryopreservation: Women receive hormonal treatment to stimulate egg production. Eggs are then removed from the follicles of each ovary, frozen, and stored until ready for use. This may be a good choice for women who do not have a partner, and who do not wish to use donor sperm to fertilize the eggs.
- Embryo freezing, or embryo cryopreservation: According to the American Cancer Society, this is the most common and successful method of preserving female fertility. It is similar to oocyte cryopreservation. In this process, the eggs are removed from a woman’s ovaries and fertilized by sperm, which has been provided by a partner or donor. The resulting embryos are frozen until ready to use.
- Pelvic shielding: Women having radiation directed to areas other than the pelvis may have their reproductive organs protected from scatter radiation by carefully placed shields.
- Removal of the cervix, or radical trachelectomy: Those with early-stage cervical cancer may have their cervix surgically removed to protect the uterus.
- Non-surgical treatment of endometrial cancer: Early-stage endometrial cancers may be successfully treated with medications instead of surgery. This can help to protect fertility.
There are also some more experimental fertility preservation techniques available to women, such as:
- Ovarian tissue cryopreservation: Ovarian tissue is surgically removed, frozen, and later implanted back into the body. It may not be suitable for those with certain cancers such as leukemia, as there may be cancer cells in the removed tissue.
- Ovarian suppression: Hormonal therapy may be used to suppress the ovaries and protect the eggs during cancer treatment.
Depending on the method of fertility preservation used and the woman’s stage in her menstrual cycle, cancer treatment may be delayed by up to 3 weeks. Some people may require immediate cancer treatment, and so not all fertility preservation methods are available to all people.
Fertility preservation options for men
Before undergoing cancer treatment, men can consider the following fertility preservation methods:
- Sperm cryopreservation: Semen samples can be frozen and stored until ready for use. These samples may be used as part of IVF treatment, or they can be thawed and placed in the uterus of a female partner. This process is known as intrauterine insemination.
- Pelvic shielding: Men having radiation treatment may have their testicles protected by carefully placed shields.
- Testicular tissue cryopreservation: This method is still being researched as a means of preserving fertility in men. Testicular tissue is surgically removed, frozen, and later implanted back into the body.
Fertility preservation options for children with cancer

Women are advised to wait for approximately 2 years after cancer treatment before becoming pregnant.
Parents of children with cancer may need to take steps to try and preserve their fertility.
Available options depend on the age of the child, whether they are pre- or post-puberty, the type of cancer treatment being considered, and the type and stage of the cancer.
Children who have entered puberty may be eligible for egg or sperm cryopreservation. Those who are prepubescent may be able to have ovarian or testicular tissue frozen.
Parental consent will be required, and consent of the children may also be necessary.
For some, fertility preservation in children may raise ethical questions. The Ethics Committee of the American Society for Reproductive Medicine advise that parents of children with cancer may act to preserve the child’s fertility if the child agrees, and if the procedure is likely to benefit the child in the future.
Effects of fertility preservation on cancer treatment
At present, there is no evidence to suggest that fertility preservation methods interfere with cancer treatment.
However, if the cancer treatment is delayed to save fertility, this may have an effect on the outcome of the cancer treatment. It is important to discuss the risk of this with a doctor.
Pregnancy after cancer treatment and fertility preservation
Successful pregnancy after cancer treatment and fertility preservation is possible. There is no evidence that cancer treatments have negative health effects on children conceived after treatment has ended. Children should not be exposed to cancer treatments while in the womb.
According to Cancer Research UK, most doctors will advise women to wait for 2 years after cancer treatment before becoming pregnant.
While pregnancy does not cause recurrence of the cancer, cancer is most likely to come back within the first 2 years after diagnosis. Women who are pregnant during this time may not be able to receive cancer treatment without risking harm to the fetus.