A new study conducted by researchers from the University of California, San Francisco, in association with the Planned Parenthood Federation of America, found that, over the course of a year, the number of unintended pregnancies was reduced “dramatically” by training health care workers to counsel young women on the benefits of intrauterine devices and contraceptive implants.
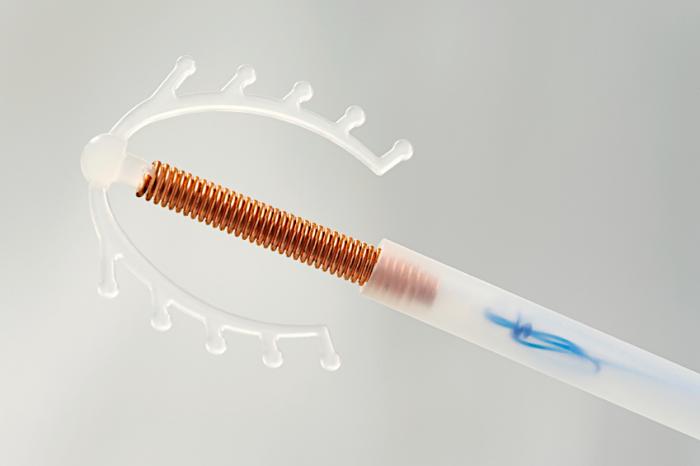
Intrauterine devices and contraceptive implants – also known as long-acting reversible contraceptives – are known to be more effective than condoms or the pill.
Forty Planned Parenthood centers across the US and 1,500 women between the ages of 18 and 25 took part in the study, published in The Lancet. The authors say that the study is the first randomized trial of a clinic-based intervention to tackle the issue of unintended pregnancies, which account for about half of all pregnancies in the country.
Though intrauterine devices (IUDs) and contraceptive implants – also known as long-acting reversible contraceptives (LARCs) – are known to be more effective than condoms or the pill, health care providers do not routinely include them in contraceptive counseling.
This is despite the American College of Obstetricians and Gynecologists recommending since 2009 that LARC methods should be used as first-line contraceptives for most women, due to their safety and high efficacy.
Previous surveys have shown that just:
- 38% of doctors in the US offer LARCs to adolescents
- 53% offer them to women without children
- 25% offer them to women after abortion.
In the new study, half of the health centers were randomly assigned to receive training in LARC counseling, while the other half continued delivering their usual care plan. The women who took part in the study were all receiving contraceptive counseling because they did not want to become pregnant in the next 12 months.
Less than 1% of LARC users become pregnant over the course of a year
The health care workers trained in LARC counseling informed women that less than 1% of women using LARCs become pregnant over the course of a year, compared with 9% of women on the pill and 18% of women whose male partners use condoms.
Overall, 71% of health care workers randomized into the intervention discussed LARC methods with their patients, compared with 39% of health care workers in the control group. The researchers found that 28% of women in the intervention group chose LARC methods, compared with 17% in the intervention group.
Among the women who attended Planned Parenthood clinics seeking family planning services following this training, unintended pregnancies fell from 15 to 8 per 100 women over the course of a year.
Given that the intervention demonstrates what would seem to be a clear benefit for LARC methods, why are they not more routinely recommended in health care?
The study authors point out that LARCs are expensive, and nearly 38% of the women in the study did not have medical insurance. However, although implant devices may cost up to $1,000, the authors point out that these methods work out cheaper than the pill over time, as they do not need to be resupplied.
Dr. Carolyn Westhoff, senior medical advisor at Planned Parenthood Federation of America, says of the findings:
“This study shows how important it is that women’s health care providers have full information about available birth control methods and are trained to provide all of these methods to patients at the same visit. It’s one very important part of making sure that women can have the birth control of their choosing – without any barriers.”
Last year, a study conducted in the UK and published in the International Journal of Women’s Health, found a correlation between a decrease in teenage pregnancies under the age of 18 between 1998 and 2011 (from 46.6 to 30.7 per 1,000 women) and an 89.7% increase in LARC usage over the same period.
Written by David McNamee